Reducing planning target volume margins decreases dose to parotid glands in head and neck cancers - a dosimetric analysis
Abstract
Introduction: Radiotherapy in head and neck cancers is treated for several weeks and daily setup and reproducibility is a challenge. This daily variability causes setup errors which accounts planning target volume margins. Reduced PTV margins have to be taken to decrease the dose to the parotid glands, without compromising on loco regional control rates. The present study is done to identify setup errors and see the feasibility to decrease the PTV margins by creating dummy radiotherapy plans in order to decrease dose to parotid glands.
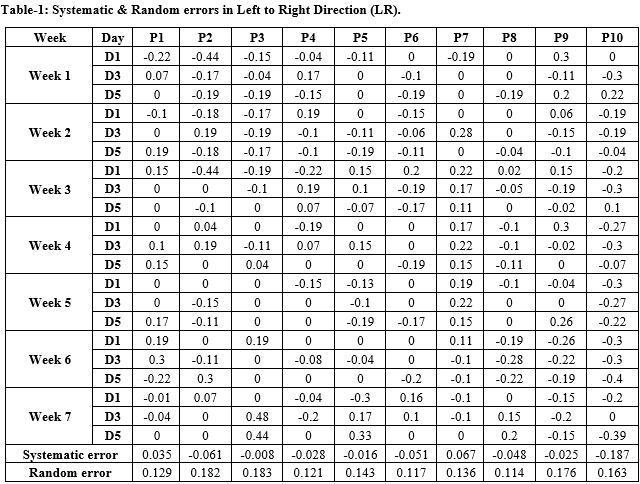
Material and Methods: 420 portal images were evaluated for setup errors in three dimensions (Antero Posterior, Left to Right and Superior to Inferior) which were performed in ten patients of oropharyngeal squamous cell carcinoma. All patients were treated in supine position using immobilization cast. After target volume delineation a PTV margin of 7mm was given. Dosimetric parameters of PTV and organs at risk were assessed. PTV margins were calculated according to three methods proposed by Stroom, Van Herk and ICRU 62. Dummy radiotherapy plans were generated using new PTV margins and compared with 7mm PTV margins. The data was analyzed using 3-way ANNOVA test for statistical significance.
Results: The optimum PTV margins were 4mm in LR and SI direction and 7mm in AP direction. The PTV parameters (V95, D95, Dmax, Dmean, HI and CI) had no significant difference among different radiotherapy plans with different PTV margins. There was a significant decrease in the dose to right parotid (39.12 Gy to 32.88Gy; p-0.04), left parotid (37.90 to 31.21Gy; p-0.03) and parotid combined (38.65 to 31.45 Gy; p-0.01) when 7mm PTV margins were reduced to 4mm PTV margins. The results of dummy radiotherapy plans using asymmetric PTV margins (LR-4mm, SI-4mm and AP-7mm) and symmetrical PTV margins (4mm in all directions) are compared with PTV margins (7mm in all directions), in terms of PTV and OAR dosimetric parameters.
Conclusion: The decreased PTV margins of 4mm decreases the dose to the parotid significantly. The implementation of radiotherapy plans needs to be supplemented by daily IGRT.
Downloads
References
Nutting CM, Morden JP, Harrington KJ, Urbano TG, Bhide SA, Clark, et al. Parotid-sparing intensity modulated versus conventional radiotherapy in head and neck cancer (PARSPORT): a phase 3 multicentre randomised controlled trial. Lancet Oncol. 2011;12(2):127-136. doi: https://doi.org/10.1016/S1470-2045(10)70290-4.
Gulliford SL, Miah AB, Brennan S, McQuaid D, Clark CH, Partridge M, et al. Dosimetric explanations of fatigue in head and neck radiotherapy: an analysis from the PARSPORT Phase III trial. Radiother Oncol. 2012; 104(2):205-212. doi: https://doi.org/10.1016/j.radonc.2012.07.005.
Lambrecht M, Nevens D, Nuyts S. Intensity-modulated radiotherapy vs. parotid-sparing 3D conformal radiotherapy. Effect on outcome and toxicity in locally advanced head and neck cancer. Strahlenther Onkol. 2013; 189(3):223-229. doi: https://doi.org/10.1007/s00066-012-0289-7. Epub 2013 Jan 16.
Radiation Therapy Oncology Group. RTOG 0022 protocol. [Internet] Available from: http://www.rtog.org/members/protocols/h0022/h0022.pdf.
Radiation Therapy Oncology Group. RTOG 0225 protocol. [Internet] Available from: http://www.rtog.org/members/protocols/0225/0225.pdf.
Radiation Therapy Oncology Group. RTOG 0435 protocol. [Internet] Available from: http://www.rtog.org/members/protocols/0435/0435.pdf.
Radiation Therapy Oncology Group. RTOG 0522 protocol. [Internet] Available from: http://www.rtog.org/members/protocols/0522/0522.pdf.
Radiation Therapy Oncology Group. RTOG 0615 protocol. [Internet] Available from: http://www.rtog.org/members/protocols/0615/0615.pdf.
Eastern Cooperative Oncology Group. ECOG 2303 protocol. [Internet] Available from: http://www.clinicaltrials.gov/ct2/show/NCT00089297.
Eastern Cooperative Oncology Group. ECOG 2399 protocol. [Internet] Available from: http://www.clinicaltrials.gov/ct2/show/NCT00014118.
The Royal College of Radiologist, Society and College of Radiographers, Institute of Physics and Engineering in Medicine. On target: ensuring geometric accuracy in radiotherapy. London: The Royal College of Radiologist. 2008:1-78.
Stroom JC, Hans CJ, Henk H, Andries VG. Inclusion of geometrical uncertainties in radiotherapy treatment planning by means of coverage probability. Int J Radiat Oncol Biol Phys. 1999;43(4):905-919. doi: https://doi.org/10.1016/S0360-3016(98)00468-4.
Van Herk M, Remeijer P, Rasch C, Lebesque JV. Theprobability of correct target dosage: dose-population histograms for deriving treatment margins inradiotherapy. Int J Radiat Oncol Biol Phys. 2000;47(4):1121-1135. doi: https://doi.org/10.1016/S0360-3016(00)00518-6.
International Commission on Radiation Units and Measurements. ICRU Report 62: Prescribing, Recording and Reporting Photon Beam Therapy. [Internet] 1999. (Supplement to ICRU Report; vol 50).
Caudell JJ, Meredith RF, Spencer SA, Keene KS, Dobelbower MC, Bonner JA. Margin on gross tumor volume and risk of local recurrence in head-and-neck cancer. Int J Radiat Oncol Biol Phys. 2010;76(1):164-168. doi: 10.1016/j.ijrobp.2009.01.037.
Dijkema T, Raaijmakers CP, Ten Haken RK, Roesink JM, Braam PM, Houweling AC, et al. Parotid gland function after radiotherapy: the combined Michigan and utrecht experience. Int J Radiat Oncol Biol Phys. 2010; 78(2):449-453. doi: https://doi.org/10.1016/j.ijrobp.2009.07.1708.
Beetz I, Schilstra C, Burlage FR, Koken PW, Doornaert P, Bijl HP, et al. Development of NTCP models for head and neck cancer patients treated with three-dimensional conformal radiotherapy for xerostomia and sticky saliva: the role of dosimetric and clinical factors. Radiother Oncol 2012;105(1):86-93. doi: https://doi.org/10.1016/j.radonc.2011.05.010.
Christianen ME, Schilstra C, Beetz I, Muijs CT, Chouvalova O, Burlage FR, et al. Predictive modeling for swallowing dysfunction after primary (chemo) radiation: results of a prospective observational study. Radiother Oncol. 2012; 105(1):107-114. doi: https://doi.org/10.1016/j.radonc.2011.08.009.
Little M, Schipper M, Feng FY, Vineberg K, Cornwall C, Murdoch-Kinch CA, et al. Reducing xerostomia after chemo-IMRT for head-and-neck cancer: beyond sparing the parotid glands. Int J Radiat Oncol Biol Phys. 2012;83(3):1007-1014. doi: https://doi.org/10.1016/j.ijrobp.2011.09.004.
Navran A, Heemsbergen W, Janssen T, Hamming-Vrieze O, Jonker M, Zuur C, et al. The impact of margin reduction on outcome and toxicity in head and neck cancer patients treated with image-guided volumetric modulated arc therapy (VMAT). Radiother Oncol. 2019;130:25-31. doi: https://doi.org/10.1016/j.radonc.2018.06.032.
Chen AM, Yu Y, Daly ME, Farwell DG, Benedict SH, Purdy JA. Long-term experience with reduced planning target volume margins and intensity modulated radiotherapy with daily image-guidance for head and neck cancer. Head Neck. 2014;36(12):1766-1772. doi: https://doi.org/10.1002/hed.23532.
Den RB, Doemer A, Kubicek G, et al. Daily image guidance with cone beam computed tomography for head and neck cancer intensity-modulated radiotherapy: a prospective study. Int J Radiat Oncol Biol Phys. 2010;76(5):1353-1359. doi: https://doi.org/10.1016/j.ijrobp.2009.03.059.
Zumsteg Z, DeMarco J, Lee SP, et al. Image guidance during head-and neck cancer radiation therapy: analysis of alignment trends with in-room cone-beam computed tomography scans. Int J Radiat Oncol Biol Phys. 2012; 83(2):712-719. doi: https://doi.org/10.1016/j.ijrobp.2011.08.001.
Yang J, Garden AS, Zhang Y, Zhang L, Dong L. Variable planning margin approach to account for loco regional variations in setup uncertainties. Med. Phys. 2012;39(8):5136-5144. doi: https://doi.org/10.1118/1.4737891.


 OAI - Open Archives Initiative
OAI - Open Archives Initiative


