Clinical spectrum of congenital heart diseases in a tertiary care hospital
Abstract
Introduction- In developing countries congenital heart diseases (CHDs) causes deaths of thousands of children. A study is necessary to understand incidence and clinical spectrum of CHDs so that early diagnosis and intervention can be done.
Material and Methods – Newborns and children up to the age of 14 years attending pediatric OPD as well as admitted in ward with CHDs enrolled for study. Data were analyzed using SPSS system version 21.
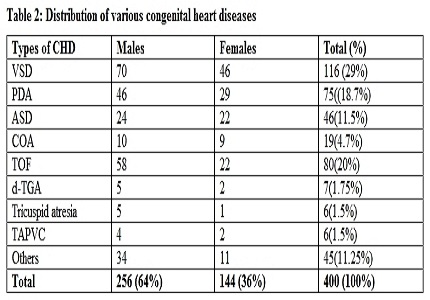
Results- A total of 400 children with CHDs included for final analysis. Male to Female ratio is 1.78:1.Most common CHDs was Ventricular septal defect followed by Tetralogy of fallot. Major symptoms were cough, difficulty in breathing, poor weight gain and suck rest suck cycle. Maternal risk factors found were consanguinity, maternal diabetes mellitus, maternal hypertension, maternal seizure disorder, maternal obesity, systematic lupus erythematosus etc.
Conclusion- VSD is most common acyanotic CHD. Males are more affected with CHDs. Consanguinity and Maternal Diabetes are important risk factors for CHDs.
Downloads
References
Schoen FJ. The Heart. In: Cortan RS, Kumar V, Robins SL, 6th ed. Robins Pathologic Basis of Disease. Philadelphia: W.B. Saunders Company, 1999; 543-600.
Hoffman JI, Kaplan S, Liberthson RR. Prevalence of congenital heart disease. Am Heart J. 2004 Mar; 147(3):425-39.doi: https://doi.org/10.1016/j.ahj.2003.05.003.
Alabdulgader AA. Congenital heart disease in 740 subjects: epidemiological aspects. Ann Trop Paediatr. 2001 Jun;21(2):111-8.
Kapoor R, Gupta S. Prevalence of congenital heart disease, Kanpur, India. Indian Pediatr. 2008 Apr;45(4):309-11.
Mohd Ashraf, J Chowdhary, K Khajuria and AM Reyaz. Spectrum of Congenital Heart Diseases in Kashmir, India. Indian Pediatr. 2009 Dec;46(12):1107-8.
Vaidyanathan B1, Sathish G, Mohanan ST, Sundaram KR, Warrier KK, Kumar RK. Clinical screening for congenital heart disease at birth: a prospective study in a community hospital in Kerala. Indian Pediatr. 2011 Jan;48(1):25-30.doi: https://doi.org/10.1007/s13312-011-0021-1.
Khali A, Aggarwal R, Thirupuram S, Arora R. Incidence of congenital heart disease among hospital live births in India. Indian Pediatr. 1994 May; 31(5):519-27.
Thakur JS, Negi PC, Ahluwalia SK, Sharma R, Bhardwaj R. Congenital heart disease among school children in shimla hills. Indian Heart J. 1995 May-Jun;47(3):232-5.
Chadha SL, Singh N, Shukla DK. Epidemiological study of congenital heart disease. Indian J Pediatr. 2001 Jun;68(6):507-10.doi: https://doi.org/10.1007/bf02723241.
Cohen AJ, Tamir A, Houri S, Abegaz B, Gilad E, Omohkdion S, Zabeeda D, Khazin V, Ciubotaru A, Schachner A. Save a child’s heart: we can and we should. Ann Thorac Surg. 2001 Feb;71(2):462-8.doi: https://doi.org/10.1016/s0003-4975(00)02243-8.
Allen HD , Lange LW, Sahn DJ ,Goldberg SJ, ultrasound cardiac diagnosis. Pediatr Clin North Am. 1978 Nov;25(4):677-706.doi: https://doi.org/10.1016/s0031-3955(16)33636-7.
Chung KJ, Simpson IA, Newman R, David JS, Frederick SS, Hesselink JR. Cine magnetic resonance imaging for evaluation of congenital heart disease: Role in pediatric cardiology compared with echocardiography and angiography. J Pediatr. 1988 Dec;113(6):1028-35.
Campbell RM, Douglas PS, Eidem BW, Lai WW, Lopez L, Sachdeva R. ACC/AAP/AHA/ASE/HRS/SCAI/SCCT/SCMR/SOPE 2014 appropriate use criteria for initial transthoracic echocardiography in outpatient pediatric cardiology. J Am Coll Cardiol. 2014 Nov 11;64(19):2039-60.doi: https://doi.org/10.1016/j.jacc.2014.08.003.
Rashid U, Qureshi AU, Hyder SN, Sadiq M. Pattern of congenital heart disease in a developing country tertiary care center: Factors associated with delayed diagnosis. Ann Pediatr Card 2016;9:210-5.doi: http://www.annalspc.com/text.asp?2016/9/3/210/189125.
Pfammatter JP1, Stocker FP. Delayed recognition of haemodynamically relevant congenital heart disease. Eur J Pediatr. 2001 Apr;160(4):231-4.
Massin MM, Dessy H. Delayed recognition of congenital heart disease. Postgraduate Medical Journal. 2006;82(969):468-70.doi: http://dx.doi.org/10.1136/pgmj.2005.044495.
Shah GS, Singh MK, Pandey TR, Kalakheti BK, Bhandari GP . Incidence of congenital heart disease in tertiary care hospital. Kathmandu Univ Med J (KUMJ). 2008 Jan-Mar;6(1):33-6.
L. Kasturi, A.V. Kulkarni, A. Amin and V.A. Mashankar. Congenital heart disease: Clinical spectrum. Indian Pediatr. 1999 Sep; 36(9):953.
van der Linde D, Konings EE, Slager MA, Witsenburg M, Helbing WA, Takkenberg JJ, Roos-Hesselink JW. Birth prevalence of congenital heart disease worldwide: a systematic review and meta-analysis. J Am Coll Cardiol. 2011 Nov 15;58(21):2241-7. doi: https://doi.org/10.1016/j.jacc.2011.08.025.
Rahman F, Salman M, Akhter N, Patwary SR, Anam K, Rahman MM, Hasan Z, Uddin MJ, Khalil MM, Hafiiz MG, Zaman SM, Fatema N, Rashid MA, Banerjee SK, Haque SS, Chowdhury NA. Pattern of congenital heart diseases. Mymensingh Med J. 2012 Apr;21(2):246-50.
Shrestha B. Nepal's noble echocardiography-database with video clips and color still images: a single individual's 6 years' experience at the Echocardiography Lab of Nepal Medical College, Teaching Hospital. Nepal Med Coll J. 2012 Sep;14(3):180-6.
Samánek M. Boy:girl ratio in children born with different forms of cardiac malformation: a population-based study. Pediatr Cardiol. 1994 Mar-Apr;15(2):53-7.doi: https://doi.org/10.1007/bf00817606.
Cameron JW, Rosenthal A, Olsan AD. Malnutrition in hospitalized children with congenital heart disease. Arch Pediatr Adolesc Med. 1995 Oct;149(10):1098-102.doi: https://doi.org/10.1001/archpedi.1995.02170230052007.
Silove ED. Assessment and management of congenital heart disease in the newborn by district pediatrician. Arch Dis Child Fetal Neonatal Ed. 1994 Jan;70(1):F71-4.doi: https://doi.org/10.1136/fn.70.1.f71.
el Hag AI. Pattern of Congenital Heart Disease in Sudanese Children. East Afr Med J. 1994 Sep;71(9):580-6.
Becker SM, Al Halees Z, Molina C, Paterson RM. Consanguinity and congenital heart disease in Saudi Arabia. Am J Med Genet. 2001 Feb 15;99(1):8-13.doi: https://doi.org/10.1002/1096-8628(20010215)99:1%3C8::aid-ajmg1116%3E3.0.co;2-u.
Ramegowda S, Ramachandra NB. Parental consanguinity increases congenital heart diseases in South India. Ann Hum Biol. 2006;33:519–28.doi: https://doi.org/10.1080/03014460600909349.
El Mouzan MI, Al Salloum AA, Al Herbish AS, Qurachi MM, Al Omar AA. Consanguinity and major genetic disorders in Saudi children: a community-based cross-sectional study. Ann Saudi Med.2008;28:169–173.
Shieh JT, Srivastava D. Heart malformation: what are the chances it could happen again? Circulation. 2009Jul 28;120(4):269-71. doi: https://doi.org/10.1161/CIRCULATIONAHA.109.878637. Epub 2009 Jul 13.
Bittles AH. A community genetics perspective on consanguineous marriage. Community Genet. 2008;11(6):324-30. doi: https://doi.org/10.1159/000133304. Epub 2008 Aug 5.
Patel SS, Burns TL. Nongenetic risk factors and congenital heart defects. Pediatr Cardiol. 2013 Oct;34(7):1535-55. doi: https://doi.org/10.1007/s00246-013-0775-4. Epub 2013 Aug 21.
LoffredoCA, WilsonPD, FerenczC.Maternal diabetes: an independent risk factor for major cardiovascular malformations with increased mortality of affected infants. Teratology. 2001 Aug; 64(2):98-106.doi: https://doi.org/10.1002/tera.1051.


 OAI - Open Archives Initiative
OAI - Open Archives Initiative


