A study to find the various causes for compressive myelopathy
Abstract
Introduction: Myelopathy was the term that describes any neurologic defect related to the spinal cord. A study was conducted to evaluate various causes of compressive myelopathy and also MR characterization of spinal cord compressive lesions.
Materials and Methods: It is a hospital-based cross-sectional study, conducted in the department of radiodiagnosis, GSL Medical College, Rajahmundry from December 2014 to August 2016. All patients referred to the department of radiology with symptoms of compressive myelopathy of the spine were included. Pre-contrast scanning was done using TiWI, T2WI, FLAIR Sagittal, STIR sagittal. A Chi-square test was used to find the statistical significance, P > 0.05 was considered to be statistically significant.
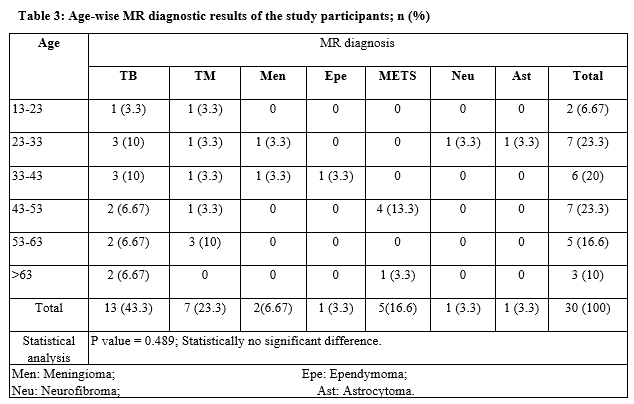
Results: During the study period total of 30 participants were included, spinal TB was diagnosed to be the most common cause of myelopathy (13; 43.3%) Extradural myelopathy was diagnosed in 23 (76.6%) participants and intradural in 7 (23.3%) members. Statistically, there was no significant difference between the age and cause for myelopathy and also between the gender.
Conclusion: The most common cause of compressive myelopathy was identified to be extradural compression form TB followed by trauma. Spinal TB was the commonest site involved. In spine injury, the common site involved was the thoracic.
Downloads
References
Matsumoto S, Hasuo K, Uchino A, Mizushima A, Kawa TF, Matsuura Y, et al. MRI of Intradural Extramedullary Spinal neurinomas and meningiomas. Clin Imaging. 1993;17(1):46-52. doi: https://doi.org/10.1016/0899-7071(93)90013-d.
Thomas J, Masary K. Neoplastic disease of the spine. Radiol Clin North Am. 1991;29(4):829-845. doi: https://doi.org/10.1067/j.cpradiol.2009.07.004.
Souweidane MM, Benjamin V. Spinal Cord Meningiomas: Neurosurgery. Clin North Am. 1994;5(2):283-291.
Li MH, Holtas S, Larsson EM. MR Imaging of Intradural Extramedullary tumors. Acta Radiol. 1992;33(3):207-212. doi: https://doi.org/10.1097/00004728-198511000-00006.
De roosa, Van Persing, Van martin E, BIoem J. MRI TB spondylitis. AJR Am J Roentgenol. 1986;147(1):79-82. doi: https://dx.doi.org/10.1177%2F2192568218769053.
Naim-ur-Rahman. Atypical forms of spinal tuberculosis. J Bone Joint Surg. 1980;62(2):162-165.
Gouliamos AD, Kehagias DT, Lahanis S, Athanassopoulou AA, Moulopoulou ES, Kalovidouris AA, et al. MR imaging of tuberculous vertebral osteomyelitis: pictorial review. Europe Radiol. 2001;11(4):575-579. doi: https://doi.org/10.1007/s003300000631.
Atlas SW. Editor. Spine and Spinal Cord. In magnetic Resonance Imaging of the Brain and Spine. Volume II; III editions: Philadelphia: Lippincott Williams and Wilkins. 2002: 1715-1972.
Sharif HAS, Morgan JL, Mona S. Role of CT and MR imaging in management of tuberculosis spondylitis. Radiol Clin North Am. 1995;33(4):787-804.
Mirvis SE, Geisler FH, Jelinek JJ, Joslyn JN, Gellad F. Acute cervical spine trauma: evaluation with 1.5-T MR imaging. Radiol. 1988;166(3):807-816. doi: https://doi.org/10.1148/radiology.166.3.3277249.
Yamashita Y, Takahashi M, Matsuno Y, Kojima R, Sakamoto Y, Oguni T et al. Acute Spinal cord Injury. Magnetic resonance Imaging correlated with myelopahty. Brit J Radiol 1991;64(759):201-209. https://doi.org/10.1259/0007-1285-64-759-201.
Kerslake RW, Jaspan T, Worthington BS. Magnetic resonance Imaging of Spinal trauma. Brit J Radiol. 1991;64(761):386-402. doi: https://doi.org/10.1259/0007-1285-64-761-386.
Flander AE, Spettell CM, Tartaglino LM, Friedman DP, Herbison GJ. Forecasting Motor Recovery after cervical spinal cord injury, value of MR Imaging. Radiology. 1996;201(3);649-655. doi: https://doi.org/10.1148/radiology.201.3.8939210.
Livingston KE, Perrin RG. The Neurosurgical management of spinal metastases causing cord and cauda equine compression. J Neuro Surg. 1978;49(6):590-594. doi: https://doi.org/10.3171/jns.1978.49.6.0839.
Smoker WRK, Godersky JC, Nutzon RK. Role of MR imaging in evaluating Metastatic Spinal disease: Amer J Roet. 1987;149(6):901-908. doi: https://doi.org/10.2214/ajr.149.6.1241.
Venkitaraman R, Sohaib SA, Barbachano Y, Parker CC, Khoo V, Huddart RA, et al. Detection of occult spinal cord compression with magnetic resonance imaging of the spine. Clin Oncol 2007;19(7):528-531. doi: https://doi.org/10.1016/j.clon.2007.04.001.
Gezen F, Kahraman S, Canakci Z, Beduk A. Review of 36 cases of Spinal cord Meningioma. Spine. 2000;25(6):727-731. doi: https://doi.org/10.1097/00007632-200003150-00013.
Gottfried ON, Gluf W, Quinones-Hinojosa A, Kan P, Schmidt MH. Spinal meningiomas: surgical management and outcome. Neurosurg Focus. 2003;14(6):e2. doi: https://doi.org/10.3171/foc.2003.14.6.2.
Koller, Gupta V, Khandelwal N, Mathuria SN, Singh P, Pathak A, et al. Dynamic magnetic resonance imaging evaluation of cranio vertebral junction abnormalities. J Comput Assist Tomogr. 2007;31(3):354-359. doi: https://doi.org/10.1097/01.rct.0000238009.57307.26.
Froment JC, Baleriaux D, Turjman F, Patay Z, Rio F. Diagnosis: neuroradiology. In: Fischer G, Brotchi J, eds. Intramedullary spinal cord tumors. Stuttgart, Germany: Thieme, 1996; 33-52.
Copyright (c) 2020 Author (s). Published by Siddharth Health Research and Social Welfare Society

This work is licensed under a Creative Commons Attribution 4.0 International License.


 OAI - Open Archives Initiative
OAI - Open Archives Initiative


